Yes, baby oral thrush can spread to mothers during breastfeeding, but it doesn’t spread like a cold or flu. It’s a Candida yeast infection, and when a baby’s mouth and a mother’s nipples stay warm and damp during feeds, the yeast can pass back and forth.
That’s why thrush can show up on both sides of nursing at the same time. If you’re dealing with sore nipples, white patches in your baby’s mouth, or feeding pain, it helps to know what’s normal, what’s not, and what needs medical care. Keep reading for the signs to watch for, how thrush spreads, when to call your doctor, and how to help stop it from coming back.
What Baby Oral Thrush Is and Why It Happens
Baby oral thrush is a yeast infection in the mouth. It happens when Candida albicans, a yeast that normally lives on the body, grows more than it should. Most of the time, Candida stays harmless. When the balance shifts, though, it can leave white patches on the tongue, gums, cheeks, or roof of the mouth.
Thrush often shows up in babies because their bodies are still learning how to keep germs in check. Their immune systems are immature, and their mouths stay warm and moist, which gives yeast a comfortable place to grow. According to the CDC’s overview of candidiasis, Candida can overgrow when the body’s normal defenses and bacteria are disrupted.
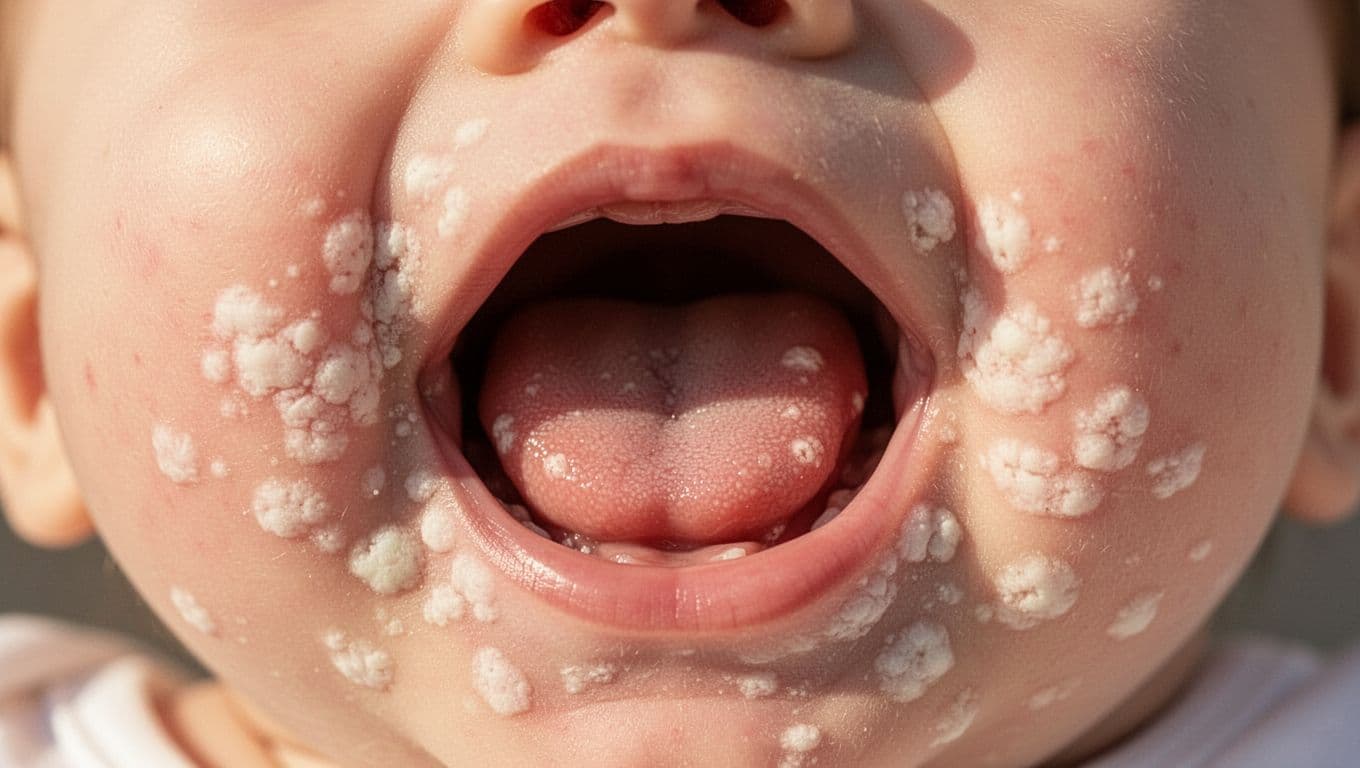
Why Candida can overgrow in a baby’s mouth
A baby’s mouth is a small, warm, damp space. That environment is ideal for yeast if the normal balance gets disturbed. When helpful bacteria drop, Candida gets more room to spread.
A few common triggers can tip that balance:
- Warmth and moisture from sucking, drooling, and feeding
- Recent antibiotics, which can lower the good bacteria that help keep yeast under control
- Pacifiers and bottle nipples that stay damp and can trap yeast
- Birth exposure, if a mother had a vaginal yeast infection during delivery
In simple terms, thrush is like a garden where one plant starts taking over after the others thin out. The yeast was already there, but the conditions changed in its favor.
Thrush is common in babies and usually treats well with the right care.
Common baby thrush risk factors parents should know
Some babies get thrush more easily than others, but many healthy babies still develop it. That can be frustrating, yet it does not mean you did anything wrong or that your baby has poor hygiene.
Risk is higher with:
- Antibiotic use, especially if your baby recently took medicine for another infection
- Frequent pacifier use, mainly if pacifiers are not cleaned well
- A vaginal yeast infection during birth, which can expose a newborn early on
- Prematurity or medical issues, such as a weaker immune system or other health concerns
Thrush can also appear more often in babies who have trouble feeding well or who spend a lot of time with moist items in the mouth. For a practical next step, you can also review home remedies for baby’s oral thrush, especially if you want to understand what gentle care may help alongside medical treatment.
How Thrush Passes Between Baby and Mother During Breastfeeding
Thrush often moves in a back-and-forth loop during nursing. A baby can pass yeast to a mother’s nipple, then pick it up again at the next feed if both are not treated.
That cycle is why breastfeeding thrush can linger. The infection stays alive in warm, moist places, so direct feeding contact gives it repeated chances to spread. According to MedlinePlus on thrush in newborns, both mother and baby often need treatment at the same time to stop reinfection.

Why breastfeeding can keep the infection going
When a baby has thrush in the mouth, the yeast can land on the nipple during nursing. If the nipple stays irritated or damp, the yeast can settle there too. Then, on the next feed, the baby’s mouth picks it up again.
That is what reinfection means in plain language. The infection does not disappear between feeds, because each nursing session can act like a handoff. For many families, this is why the soreness seems to improve, then come right back.
This is also why cracked nipples matter. Broken skin gives yeast an easier place to grow, and the cycle can start over fast. If nipple pain is already part of the picture, breastfeeding mistakes that can worsen nipple pain can be a helpful next read.
Can mothers pass thrush back to their baby?
Yes, mothers with nipple thrush can pass it back to the baby during nursing. The baby’s mouth touches the infected skin, and the yeast moves in the same way it did before.
Treating only one person often leads to the infection returning. The baby may get better for a short time, then become infected again from the mother. The same can happen in reverse if the mother is treated but the baby is not.
That is why doctors usually treat both mother and baby together. It breaks the cycle instead of chasing the infection from one person to the other.
If only one side gets treated, thrush often comes back after a few feeds.
What thrush does not usually spread through
Thrush is not usually spread by coughing, sneezing, kissing, or normal skin contact. It spreads much more easily through direct contact during breastfeeding, or through items that stay in the baby’s mouth.
That can be reassuring. You do not need to treat thrush like a cold or worry about casual contact in the house. Hugging, sharing a room, and normal family contact are not the usual problem.
Still, good hygiene helps during treatment. Clean pacifiers, bottle nipples, and anything else that goes in the baby’s mouth. Also, wash hands well after feeds and diaper changes so the yeast has fewer chances to move around.
Signs of Thrush in Babies and Mothers
Thrush often shows up in a few clear ways, but the signs can look different in a baby and a breastfeeding mother. A baby may seem only a little bothered, while the mother feels sharp nipple pain or a burning ache that makes feeds miserable.
Spotting the pattern early matters. If both of you have symptoms at the same time, thrush becomes more likely, especially when feeding pain keeps coming back.
What oral thrush looks like in babies
In babies, oral thrush usually shows up as white patches on the tongue, gums, inside the cheeks, or the roof of the mouth. These patches often look creamy or curd-like, and they do not wipe away easily with a soft cloth.

Some babies seem comfortable, while others get fussy during feeds. You may notice pulling off the breast or bottle, crying more than usual, or refusing to feed because sucking hurts.
Other signs can include:
- White patches that stay in place
- Red or sore areas under the patches if they rub off
- Feeding fussiness or short, interrupted feeds
- Diaper rash in some babies, since yeast can affect more than one area
A white tongue alone is not always thrush, since milk residue can look similar. The clue is whether the spots spread beyond the tongue and stay stuck to the mouth.
How nipple thrush feels for breastfeeding mothers
For mothers, nipple thrush often feels like burning, itching, or stabbing pain during or after nursing. The nipples may look red, shiny, flaky, or irritated, and the skin can feel extra sensitive to touch.
The pain can start as soon as the baby latches, then linger between feeds. In some cases, the discomfort spreads deeper into the breast, which can feel like a burning or shooting ache.
Common symptoms include:
- Nipple pain during feeds
- Burning or itching on the nipple or areola
- Shiny, red, or flaky skin
- Deep breast soreness in some cases
If nipple pain keeps getting worse instead of better, it deserves attention. Persistent breast pain should not be brushed off, especially when feeding is involved, and persistent breast pain needs evaluation can help explain why.
When thrush is involved, the pain often feels sharp, sore, and out of proportion to a normal latch issue.
When symptoms may look like something else
Thrush does not always have a neat, textbook look. Cracked nipples, latch problems, and eczema can overlap with it, so the symptoms can blur together fast.
A bad latch can cause sore nipples. Eczema can cause dryness, flaking, and redness. Cracks from feeding can also make the skin burn and sting, which feels a lot like thrush.
That is why a clinician may need to check before treatment starts. If the signs are unclear, getting the right diagnosis helps you avoid treating the wrong problem and keeps the infection from dragging on.
How Doctors Diagnose Thrush and When You Should Get Help
Doctors usually diagnose thrush with a visual exam first. That means they look closely at your baby’s mouth and, if you’re breastfeeding, at your nipples too. In many cases, that is enough to make the call, especially when the signs line up with feeding pain and a classic white patch pattern.
What a doctor looks for during an exam
A doctor checks for white, creamy patches inside the baby’s mouth. These spots usually sit on the tongue, cheeks, gums, or roof of the mouth, and they do not wipe away easily. If the area underneath looks red or sore, that adds more support for thrush.
On the mother’s side, the exam focuses on the nipples and areola. Doctors look for redness, shiny skin, flaking, cracks, or bleeding, along with a pain pattern that feels burning, stabbing, or worse after feeds. They also ask about feeding, because babies with thrush may pull off the breast, fuss more, or refuse to latch.
According to Mayo Clinic’s guidance on oral thrush, testing is not always needed when the exam is clear. Still, if the picture is messy or symptoms keep coming back, a clinician may want a swab or another check to rule out a different cause.
Red flags that mean you should not wait
Call a doctor sooner if pain keeps getting worse, feeding becomes a struggle, or treatment does not help. You should also get help fast if your baby has fever, poor weight gain, refusal to feed, or signs of dehydration.
For mothers, bleeding nipples, repeated thrush, or symptoms that return after treatment are also warning signs. If the same pain keeps cycling back, the problem may not be simple thrush, so it needs another look.
If symptoms worsen instead of easing, do not wait for them to clear on their own.
The safest move is to get checked early, then treat both baby and mother if thrush is confirmed.
Treatment Works Best When Mother and Baby Are Treated Together
When thrush shows up during breastfeeding, the usual fix is to treat both people at the same time. That matters because yeast can move back and forth during feeds, so treating only one side often leaves the other side ready to send it back.
The goal is simple: clear the infection in the baby’s mouth, calm the mother’s nipples, and break the cycle before it starts again. In many cases, breastfeeding can continue while treatment is underway, as long as the doctor has confirmed the plan.

Common treatments for babies with oral thrush
For babies, doctors often prescribe a liquid antifungal medicine that goes directly into the mouth, usually nystatin. It coats the infected areas and helps clear the yeast where it grows, which is why timing and dose matter so much.
Using it exactly as directed is key. If you skip doses, stop early, or give less than prescribed, the infection can hang around and come back fast. Even if the mouth looks better in a few days, the medicine usually needs to keep going for the full course.
A doctor may also give simple instructions like:
- Place the medicine where the white patches are
- Use it after feeds, if directed
- Keep pacifiers and bottle nipples clean during treatment
The NHS notes that oral thrush in babies is often treated with an antifungal liquid or gel, and careful handwashing matters too. That extra step helps stop yeast from moving right back into the mouth.
Common treatments for breastfeeding mothers
For mothers, treatment usually starts with an antifungal nipple cream applied to the nipple and areola after feeds. If symptoms are more intense, or if the infection keeps coming back, a doctor may also prescribe oral antifungal medicine.
The right choice depends on how bad the symptoms are. Mild nipple irritation may need a cream only, while deeper pain or repeated thrush may need stronger treatment. A clinician will match the medicine to the symptoms, feeding history, and how long the problem has been going on.
According to Mayo Clinic’s guidance on oral thrush, nipple symptoms can include redness, cracking, shiny skin, and pain during feeds. When those signs show up, the mother usually needs treatment alongside the baby.
Why treating only one person often fails
Thrush acts like a loop. The baby passes yeast to the nipple, then the nipple passes it back to the baby at the next feeding. If only one person gets treated, the other person can keep the infection alive.
That is why both treatments need to happen during the same window. Starting together gives the yeast fewer places to hide, and it lowers the chance of the symptoms disappearing and then returning a few days later.
A simple way to think about it is this:
- Treat the baby’s mouth.
- Treat the mother’s nipples.
- Keep both treatments going for the full time prescribed.
When both sides get treated at once, the infection has a much harder time bouncing back.
Simple Home Care Habits That Help Thrush Heal Faster
Medical treatment does the main work, but daily habits can make healing smoother and help keep thrush from bouncing back. Small details matter here. Moisture, dirty feeding gear, and irritated skin give yeast a place to linger, so simple cleanup and dry skin care can help break that cycle.
Keep nipples dry and clean after feeds
Yeast loves warm, damp skin. After nursing, gently pat the nipple area dry with a clean towel or soft cloth, then let it air out before putting your bra back on. That small pause helps because trapped moisture can keep the skin irritated and give yeast a better place to grow.
Change breast pads often, especially if they feel damp. If you use reusable pads, wash them well and let them dry fully before the next use. Clean, dry skin heals better than skin that stays wet all day.
Clean bottles, pacifiers, pump parts, and nipple shields
Anything that goes in the baby’s mouth can hold yeast. That includes bottles, pacifiers, pump parts, and nipple shields. Wash these items well after each use, and let them dry completely, because leftover moisture can keep yeast alive.
The NHS recommends washing and sterilizing dummies, teats, and other mouth items during thrush treatment, along with thorough handwashing after diaper changes and feeds. NHS breastfeeding thrush guidance gives a practical checklist that fits well into everyday care.

A quick routine helps:
- Wash feeding items right after use.
- Rinse away any soap.
- Dry them fully before storing.
Support a good latch and healing nipples
A shallow latch can rub the nipple and make cracked skin worse. Damaged skin hurts, and it also gives yeast an easier opening. If nursing feels sharp, pinchy, or keeps getting worse, the latch may need a closer look.
A lactation consultant can help you adjust positioning and make feeds less painful. If you need more support with latch and milk flow, better latch and milk supply tips can be a helpful next step.
If the pain keeps returning, don’t just push through it. Sore nipples need support so they can heal.
Good handwashing matters too, especially after diaper changes and before feeds. Together, these habits lower the chance of reinfection and give treatment a better chance to work.
How to Lower the Chance of Thrush Coming Back
Thrush can come back when treatment stops too soon or when yeast still has a place to grow. The good news is that a few simple habits can lower that risk a lot. Focus on finishing medicine, keeping feeding items clean, and watching for signs that the nipples or baby’s mouth still need attention.

Finish treatment even if symptoms improve early
It’s easy to feel relieved when the white patches fade or the nipple pain eases. Still, stopping medicine early can leave yeast behind. That leftover yeast can grow back fast, which is why symptoms often return a few days later.
Follow the full treatment plan, even if things look better before the last dose. If your doctor prescribed medicine for both you and your baby, both courses need to finish. That keeps one side from re-seeding the other.
A few habits help here:
- Take or give every dose on schedule.
- Keep using the medicine for the full time prescribed.
- Don’t switch to another product unless your doctor says to.
Watch for repeat infections and treat them early
If thrush keeps coming back, get a follow-up visit. Recurrent symptoms can mean the latch still needs work, there’s leftover infection, or something else is causing the pain. A clinician may want to check for nipple damage, a shallow latch, or a different skin issue.
Early treatment matters because yeast spreads easier when the skin is cracked or moist. Clean pacifiers, pump parts, and bottle nipples well, and keep nipples dry after feeds. The USDA breastfeeding thrush guidance also notes that both mother and baby often need care at the same time to stop the cycle.
If soreness, white patches, or burning pain returns, don’t wait it out. The sooner you treat it, the easier it is to stop another round.
Conclusion
Yes, baby oral thrush can pass to mothers during breastfeeding, and mothers can pass it back again. The good news is that it usually clears with the right antifungal treatment and simple hygiene steps.
The biggest takeaway is to spot the signs early, then treat both baby and mother together if a doctor confirms thrush. That helps break the cycle, eases feeding pain, and lowers the chance of it coming back.
If symptoms are severe, keep returning, or make feeding hard, get medical advice quickly. Parents do not need to panic, they just need to act early and stay consistent with treatment.
Save pin for later

- Baby White Tongue: When to Worry and Call the Doctor - May 5, 2026
- Is Baby Oral Thrush Contagious to Mothers? Signs and Treatment - May 5, 2026
- Can Formula Cause White Coating on Baby’s Tongue? - May 5, 2026