You do not need to do everything perfectly to feed your baby well. In the first days and weeks, breastfeeding and pumping can feel like a lot, especially when you’re tired, sore, and trying to learn your baby’s cues at the same time. Early feeding often means 8 to 12 sessions in 24 hours, whether you’re nursing, pumping, or doing both, so even simple choices can start to feel big.
The good news is that the right basics, a comfortable setup, and a little support can make those long days easier. Your recovery matters too, and if birth healing is part of the picture, healing after C-section delivery can affect how you sit, hold your baby, and manage feeds. This guide will help you get started, build confidence, and know when it’s time to ask for help instead of trying to push through on your own.
Start with the basics that make feeding easier
In the first days and weeks, the biggest wins usually come from simple, repeatable basics. Feeding often, watching your baby instead of the clock, and getting a comfortable latch matter more than buying extra gear.
That early stretch is a lot of learning at once. Your baby is learning how to feed, and your body is learning how much milk to make. Small things done often usually help the most.
How often newborns usually feed, and why that matters
Most newborns feed 8 to 12 times in 24 hours, and some want to nurse even more often for short stretches. That pattern is normal in the early weeks because frequent feeding and milk removal tell your body, “make more milk.” The more often milk is removed, whether by baby or pump, the stronger that message tends to be.
According to the CDC’s breastfeeding frequency guidance, many babies feed every 1 to 3 hours, day and night. That can feel nonstop at first, but it is often part of building supply, not a sign that something is going wrong.
Cluster feeding can also catch parents off guard. Your baby may want to nurse again and again over a few hours, often in the evening. That does not automatically mean low milk supply. Sometimes babies cluster feed during growth spurts, or when they want extra comfort and closeness.
A few simple expectations can make those early days feel less confusing:
- Newborn feeding is often frequent and uneven, not neatly spaced.
- One long stretch does not set the pattern for the whole day.
- Feeding on cue usually works better than trying to force a strict schedule right away.
If your baby is feeding often and you are also trying to rest, keep your setup easy. Water nearby, a pillow that helps, and a spot where you can settle in matter more than extra gadgets.
What a good latch looks and feels like
A good latch is usually a deep latch, not a baby hanging on just the nipple. In plain terms, your baby’s mouth should open wide, take in a good amount of breast, and stay close to the breast during the feed.
Look for a few common signs. The mouth is wide open, the lips are flared outward, and the chin presses into the breast. You will often see more areola above the top lip than below the bottom lip. Sucking should look steady, and you may hear or see swallowing after the first quick sucks.

How should it feel? Usually, you will feel tugging and pressure, especially at first, but feeding should not stay sharply painful. Ongoing pinching, toe-curling pain, or nipple damage often points to a shallow latch.
Common signs a latch needs work include:
- Clicking sounds during feeds
- Nipples that look creased or flattened after nursing
- Pinching, rubbing, or sharp pain
- Baby slipping off the breast often
A deep latch usually protects your nipples and helps your baby transfer milk better.
If pain keeps happening, get help early. Even one small position change can make a big difference. The CDC’s breastfeeding basics page also explains what early feeding and latch practice can look like.
When skin-to-skin and feeding cues can help more than the clock
Feeding usually goes more smoothly when you catch early hunger cues. Before crying starts, many babies show you they are ready by stirring, turning their head, opening their mouth, rooting, or sucking on their hands. These signs are often easier to work with because your baby is still calm.
The CDC’s hunger cue guide notes that crying is often a late hunger sign. Once a baby is upset, latching can be harder. That is why watching your baby often works better than watching the clock alone.
Skin-to-skin can help here, too. Holding your baby against your bare chest can calm both of you, wake up feeding instincts, and make it easier to notice those early cues. It can also support milk production because frequent closeness often leads to more feeding and more milk removal. If you want more ideas for skin-to-skin contact with your newborn, gentle bonding time can fit right into your feeding routine.

A practical rhythm in the early weeks often looks like this: keep baby close, notice stirring or hand sucking, offer the breast, and feed often. That simple cycle can do more for early success than a strict timer.
Choose breastfeeding and pumping essentials that are actually useful
When you’re building your feeding setup, the goal is simple: buy the items that make daily life easier, then stop. You don’t need a huge stash or a cart full of gadgets. A few well-chosen basics can save your nipples, your time, and your energy.
Breastfeeding supplies worth having in the early weeks
A small group of basics usually goes much further than a long shopping list. Soft nursing bras make frequent feeds easier, and breast pads help with leaks once your milk comes in. If your skin gets sore, a simple nipple cream can make those first latch-heavy days more manageable.

You’ll also get real use from burp cloths and a large water bottle. Both tend to stay in constant rotation. A supportive pillow can help, too, especially if your back, shoulders, or incision area needs extra comfort during longer feeds.
Some moms like a basic feeding tracker, whether it’s a notebook or an app, just to keep tabs on feeds and diapers in the foggy newborn stage. Still, you do not need every item on this list. If latch is going well and you’re comfortable, keep it simple. For more comfort tips, proper support and care for nursing breasts can help you avoid a few common mistakes.
Pumping gear that can save time and stress
If you’re pumping at all, start with a reliable pump that fits your routine. Then focus on the parts that affect comfort and output. The biggest one is the flange, because pumping should not hurt, and poor fit can make milk removal less effective.
A few practical add-ons make a real difference:
- Milk storage bags or bottles give you an easy way to save pumped milk.
- Extra pump parts let you rotate clean sets instead of washing the same pieces all day.
- A hands-free pumping bra can free up your hands for a snack, a text, or bottle prep.
- A cooler bag helps if you’ll pump at work, in the car, or away from home.

If you’re trying to avoid overspending, skip duplicate gadgets first. Put your money into a pump that works well and parts that fit well. Even Parents’ guide to breastfeeding basics makes the same point: a short list of useful supplies beats a pile of “just in case” purchases.
Why flange fit and pump setup matter more than many moms expect
A good flange fit is more important than most first-time moms realize. Your nipple should move freely in the tunnel during pumping. It should not rub hard against the sides, and the pump should not pull in too much areola.
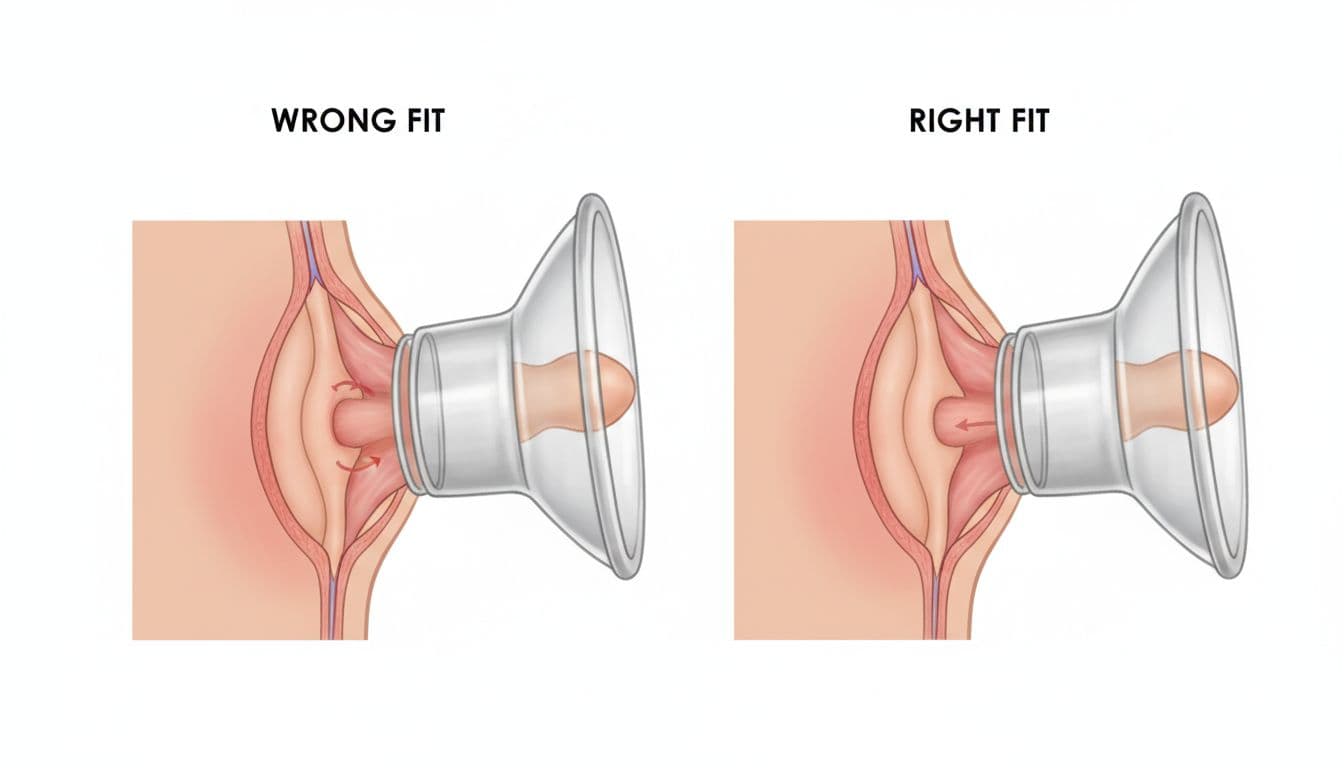
When the flange is too small or too large, you may notice pain, pinching, swelling, or less milk than expected. Over time, the wrong size can lead to poor milk removal, which may lower output. If pumping feels sharp, frustrating, or oddly inefficient, flange fit is one of the first things to check.
If pumping hurts every time, don’t assume you just need to tough it out.
Start by rechecking your flange size, centering the nipple before suction starts, and using the lowest setting that removes milk well. If you want a clear visual guide, Cleveland Clinic’s flange sizing advice is a helpful place to start.
Build a simple feeding and pumping routine that fits real life
A feeding routine should support your day, not run it. In the early weeks, the main goal is regular milk removal, because that is what helps build and protect supply. The exact pattern can look different if you’re exclusively breastfeeding, exclusively pumping, or combining both.
Direct nursing means your baby removes milk at the breast. Exclusive pumping means the pump does that job for every feed. Combo feeding sits in the middle, with some feeds at the breast and some by pump or bottle. Different setups can work well, as long as your routine keeps up with your baby’s needs and your body’s milk-making rhythm.
A realistic breastfeeding and pumping rhythm for the early weeks
In the beginning, many moms pump every 2 to 3 hours, including overnight, if they are establishing supply or replacing missed feeds. That often adds up to 8 to 12 milk removals in 24 hours, whether the milk comes out by baby, pump, or both. The clock can help at first, but your body still responds best to steady milk removal.
If you’re exclusively pumping, staying fairly close to that rhythm matters most in the first weeks. Skipping long stretches too early can make supply harder to build. The CDC’s breast milk pumping guidance also points parents toward frequent pumping early on, especially when baby is not nursing well or is away from you.
If you’re directly nursing, your routine may look looser. Some moms pump after a few feeds, often in the morning, to build a small freezer stash or to increase supply. Others only pump when they are separated from baby. Both are normal. It depends on your goal, not on what someone else posts online.
A simple way to think about it is this:
- If baby nurses well and is with you most of the day, you may not need to pump much.
- If a bottle replaces a feed, pumping around that time usually helps protect supply.
- If you’re trying to boost output, adding regular pumping sessions can help.
A good routine is one you can repeat while tired, healing, and living real life.
You may also want to leave space for recovery. If you’re still sore after birth or managing incision pain, keeping feeds and pump sessions comfortable matters just as much as timing. Small setup changes, like better back support or easier seating, can help, especially during C-section recovery and newborn care.
How to pump step by step for better comfort and output
Good pumping is less about turning the suction high and more about using a setup your body responds to. A few small steps can make pumping feel better and work better.
Start with this basic flow:
- Wash your hands and make sure your pump parts are clean and dry.
- Center the flange so your nipple sits in the tunnel and can move freely.
- Begin with a fast, gentle setting to trigger let-down.
- After milk starts flowing, switch to a slower setting with suction that feels strong but still comfortable.
- Use breast massage or gentle compression during the session to keep milk moving.
- Pump for about 15 to 20 minutes, or until milk slows and the breasts feel softer.

If pumping hurts, pause and check your flange position and suction level. Pain is often a sign that something needs adjusting. A helpful rule is to use the lowest suction that removes milk well, not the highest one you can tolerate.
Double pumping, which means pumping both breasts at the same time, is often the easiest option. It saves time, and many moms get better output because both breasts are stimulated together. That can be especially useful when you’re pumping often or fitting sessions around naps, diaper changes, and meals.
Warmth can help too. Some moms get a better let-down after a warm shower, a warm compress, or a few minutes of hand massage first. If you want a few more examples of how moms build a flexible plan, Healthline’s sample pumping schedules can give you a practical starting point without making it feel rigid.
Simple sample schedules for nursing, combo feeding, and going back to work
Sample schedules are best used as templates, not rules. Your baby may eat sooner, later, or more often on some days. That’s normal. The point is to keep milk moving and make your routine easy to repeat.
Here are a few realistic examples:
- Mostly nursing at home: Nurse on demand through the day and night, then pump once after the first morning feed if you want extra milk for storage. Morning output is often higher, so that one session may give you the most for the least effort.
- Combo feeding: Nurse during the day when you’re together, then pump after 1 or 2 feeds or whenever a bottle replaces a nursing session.
- Back at work: Nurse before leaving, pump about every 3 hours while away, then nurse again when you’re back with baby.

A workday rhythm might look like a nurse before daycare drop-off, a pump mid-morning, another at lunch, and one more in the afternoon. Then you nurse again at home. The Cleveland Clinic’s back-to-work pumping schedule offers similar examples, and it can help if you want to picture how sessions fit into an actual workday.
Some days will go off plan. Baby may cluster feed. You may miss a pump. You may get more milk at 6 a.m. than at 3 p.m. None of that means your routine failed. It usually means you’re feeding a baby, not following a spreadsheet.
Solve common breastfeeding and pumping problems before they snowball
Small feeding problems can grow fast when you’re tired and trying to push through. The good news is that many early issues improve with a few simple changes, especially when you catch them early. This section is here to help you spot what is common, try safe basics at home, and know when it’s time to get extra support.
What to do when feeding hurts or baby will not latch well
Some nipple tenderness can happen at first, but ongoing pain is a sign to pause and fix the cause. Breastfeeding should not feel like you have to brace yourself every time your baby latches. If pain lasts through the feed, your nipples look creased after nursing, or your baby keeps slipping off, the latch likely needs work.
Start with position. Bring your baby in close, tummy to tummy, with their head, shoulders, and hips lined up. Then wait for a wide-open mouth and aim the nipple toward the roof of the mouth, not straight into the center. A deep latch usually feels like pulling and pressure, not pinching.
A few simple changes often help:
- Feed before baby gets very upset, because a frantic baby usually latches worse.
- Try skin-to-skin time for a few minutes first, since it can calm both of you.
- If your breasts feel very full, hand express a little milk first to soften the area.
- Change positions, such as laid-back or side-lying, if one hold keeps hurting.
If pain keeps happening, get help early. The La Leche League sore nipple guide and Cleveland Clinic’s latch overview both explain what a deeper latch should look and feel like. A lactation consultant can also check for issues like tongue-tie, weak suck, or breast fullness that makes latching harder.
If breastfeeding hurts every time, don’t treat that as normal. Early help is often the fastest fix.
How to handle low output, missed sessions, and worries about supply
Low pump output can feel alarming, but pumped ounces do not always show your full milk supply. Many babies remove milk better than a pump does. Time of day, stress, flange fit, missed sessions, and even how relaxed you are can change what you see in the bottle.
If output dips, first look at the pattern, not one session. Missing a pump once does not ruin your supply. Still, repeated long gaps can tell your body to make less milk, so getting back to regular milk removal matters.
These steps usually help the most:
- Pump or nurse more often for a few days.
- Make sure your breasts feel well-drained, not just lightly pumped.
- Use hands-on pumping, with gentle massage and compression during the session.
- Drink enough water and eat regularly, because running on empty makes everything harder.
- Rest when you can, since heavy fatigue and stress can affect letdown.
- Try power pumping once a day for a few days if you need a short-term boost.
The CDC’s pumping guidance recommends matching pumping frequency to how often your baby feeds when you’re apart. If you want a clear reminder that pump output is not the whole story, KellyMom’s low milk supply guide is helpful and reassuring.
If your baby has fewer wet diapers, poor weight gain, or feeds that always seem ineffective, get skilled help instead of guessing. That is also a good time to look at comfort issues outside feeding, because stress can stack up fast in the newborn stage. If your body is still healing, postpartum recovery basics after a C-section may help you make feeds and pumping sessions less draining.
Ways to prevent engorgement, clogged ducts, and extra stress
Engorgement often starts when milk sits too long and the breasts get overly full, firm, and hard to latch onto. Clogged ducts can follow when milk is not moving well. The simplest prevention is also the least glamorous: remove milk regularly and do not go too long between feeds or pumps.
That matters even more in the early weeks, when your body is still figuring out supply. If you know you’ll miss a feeding, pumping around that time can help. Also, wear a non-restrictive bra and avoid anything that puts steady pressure on the breast, including tight straps or sleeping positions that press on one area for hours.
Relief should stay gentle. Light massage, warmth before feeding, and cold packs after can help with comfort. If the breast is too full for baby to latch, hand express just enough to soften the areola. For more detail, the HealthyChildren engorgement guide and Cleveland Clinic’s clogged duct page cover basic home care.
Watch for signs that need medical care, because a clog can turn into mastitis:
- Fever
- Redness that spreads
- Flu-like body aches
- Worsening pain
- A hard area that does not improve
If those signs show up, call your doctor promptly. You do not need to wait until you feel miserable. Early treatment can protect your health and make feeding easier again.
Protect your milk, your time, and your peace of mind
A feeding plan works better when it protects more than supply. It should also protect your time, lower stress, and make the day feel less chaotic. A few simple habits can help you store milk safely, clean pump parts the right way, and stay steady when the routine starts to wear on you.
Breast milk storage and pump cleaning basics every mom should know
Safe storage matters because pumped milk is only helpful if it stays safe to use. The easiest rule is to follow current CDC breast milk storage guidance for room temperature, fridge, and freezer timing. Right now, that means freshly expressed milk can stay at room temperature for up to 4 hours, in the fridge for up to 4 days, and in the freezer for about 6 months for best quality, or up to 12 months if needed.
Keep it simple from the start. Label each container with the date, and if your baby goes to daycare, add your baby’s name if needed. It also helps to store milk in small portions, often 2 to 4 ounces, so you thaw only what your baby will likely drink.
A few storage habits save a lot of waste later:
- Put milk in the back of the fridge or freezer, not in the door.
- Cool fresh milk before adding it to already chilled milk, if you’re combining batches.
- Use thawed milk within 24 hours in the fridge, and don’t refreeze it.
- Use leftover milk from a feeding within 2 hours.
Cleaning matters just as much. After each pump session, handle parts carefully, wash them as directed, and let them air-dry fully on a clean surface. Bottles, flanges, valves, and membranes all need attention because milk residue can hide in small corners.
If you want the full article to go deeper, this is the place for a quick-reference chart and CDC-based timing notes. Keep that part practical and easy to scan, because no mom wants to decode storage rules while holding a crying baby and a full bottle.
When you’re tired, a clear label and a clean pump set can feel like future-you came to help.
How to make pumping more manageable during busy days
Busy days fall apart when every pump session requires five decisions first. A small routine fixes that. The goal isn’t perfection, it’s fewer moving parts.
Start the night before. Pack your pump parts, charger, bottles, storage bags, and cooler bag before bed. Add a spare shirt and breast pads, too, because leaks always seem to happen when you’re already late.
Then reduce the mental load with a few repeatable habits:
- Set alarms for your usual pump times so you don’t have to keep checking the clock.
- Keep one small bag stocked with your pumping basics.
- Use a simple note in your phone to track time and ounces.
- Restock that bag as soon as you get home, not the next morning.
That last step matters more than it sounds. Morning-you is usually rushed, and rushed moms forget valves, bottles, or the one clean flange set they thought was in the bag.
A simple log can also help you spot patterns without turning feeding into homework. You don’t need a detailed spreadsheet. Just jot down the time, amount pumped, and anything unusual, such as pain, a missed session, or a longer stretch of sleep. If your output dips, those notes can show why.
If you’re heading back to work or managing errands all day, Cleveland Clinic’s pumping-at-work tips are useful because they focus on practical scheduling, not pressure. The more automatic your routine feels, the less energy you waste making the same choices over and over.
When to ask for help, and why support can change everything
Some feeding issues improve with time. Others need real support. Asking for help early can save you pain, protect milk supply, and ease a lot of worry.
Reach out to a lactation consultant, your pediatrician, or your OB-GYN if your baby isn’t feeding well, diaper counts seem low, weight gain is a concern, or pain keeps going. The same goes for cracked nipples, repeated clogged ducts, or pump sessions that always feel miserable. Those are signs to check the setup, not signs that you should push through.
A good support team can help with things like:
- Latch problems
- Poor milk transfer
- Low pump output
- Ongoing breast or nipple pain
- Feeding plans after birth complications or separation from baby
Many moms wait too long because they think they should be able to figure it out alone. That pressure helps no one. Getting support is common, and it’s smart. Even one appointment can make feeding feel more doable.
If you need help knowing when to reach out, this guide on when to see a lactation consultant can help you spot the signs sooner. Support also matters for your mental load. When someone helps you make a plan, pumping and feeding stop feeling like a test you have to pass and start feeling like a routine you can actually live with.
Sometimes consistency comes from gear and timing. Just as often, it comes from hearing, “You’re not doing this wrong, you just need support.”
Conclusion
Breastfeeding and pumping usually take some trial and error, and that is completely normal. Most moms do best when they focus on the basics, a comfortable latch or pump setup, frequent milk removal, and a few essentials that make daily feeding easier.
Progress rarely looks perfect in the early weeks, because babies change fast and your body is still learning, too. Still, simple routines, good flange fit, safe milk storage, and early help for pain or low output can make a big difference and prevent small issues from turning into bigger ones.
Most importantly, your feeding plan can change as your baby grows. You can nurse more, pump more, combine both, or adjust your routine to fit work, sleep, recovery, and real life, while still doing a good job for your baby.
Save the pin for later

- 100 Funny Baby Jokes That Will Make You Laugh - May 15, 2026
- Baby Rolling Eyes: Causes, Symptoms, and When to Worry - May 15, 2026
- How Long Can a Baby Go Without Pooping? - May 15, 2026





